Diagnosis
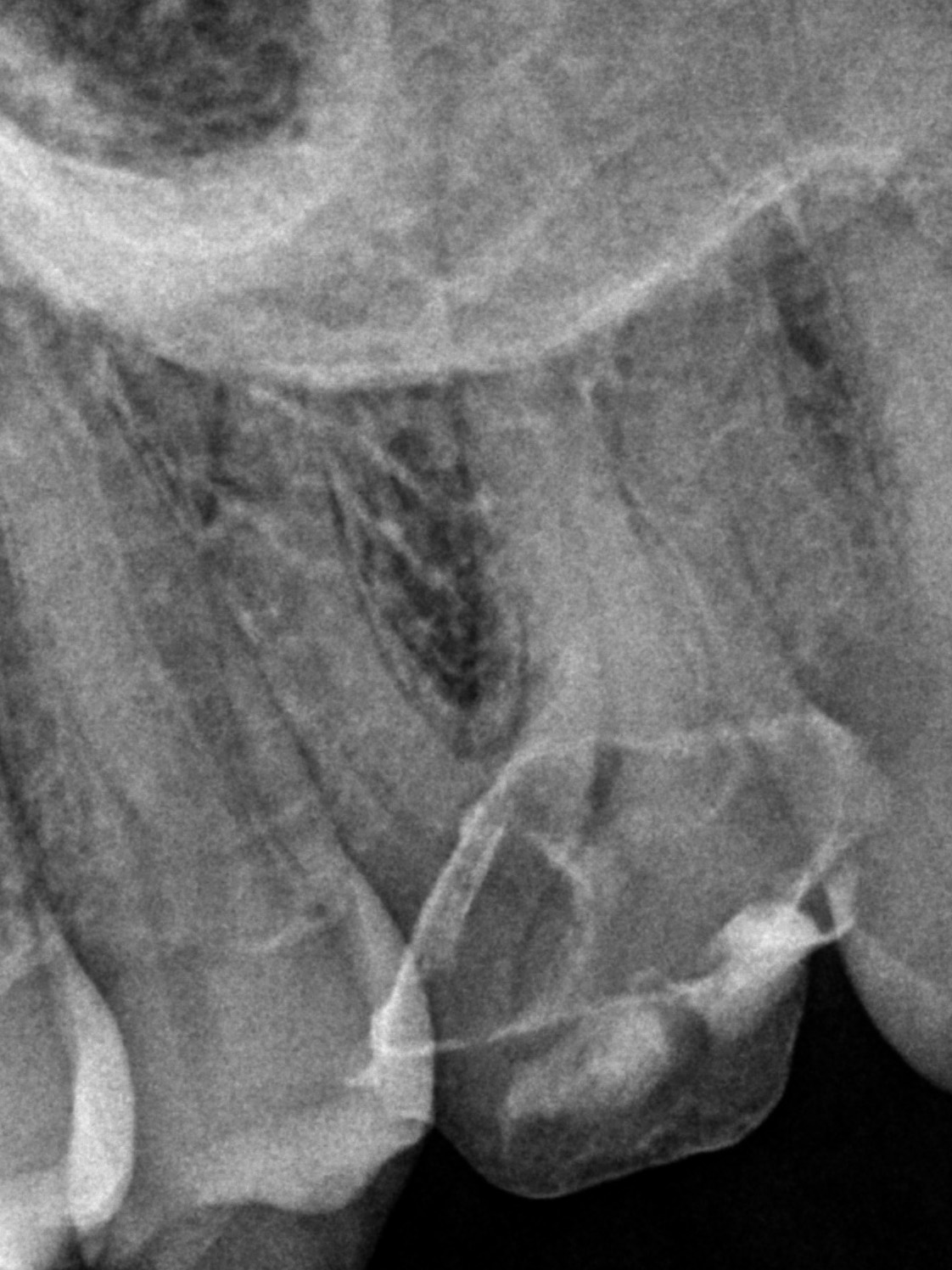
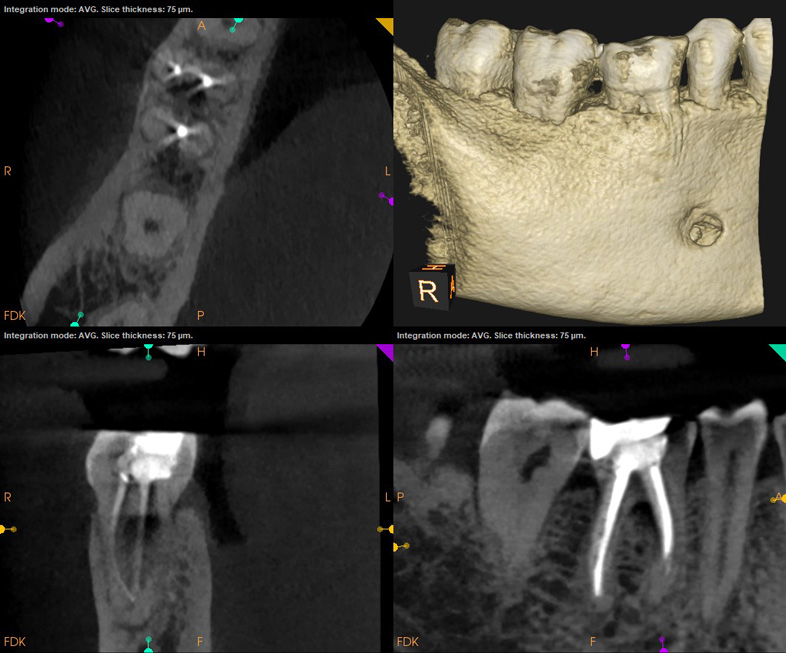
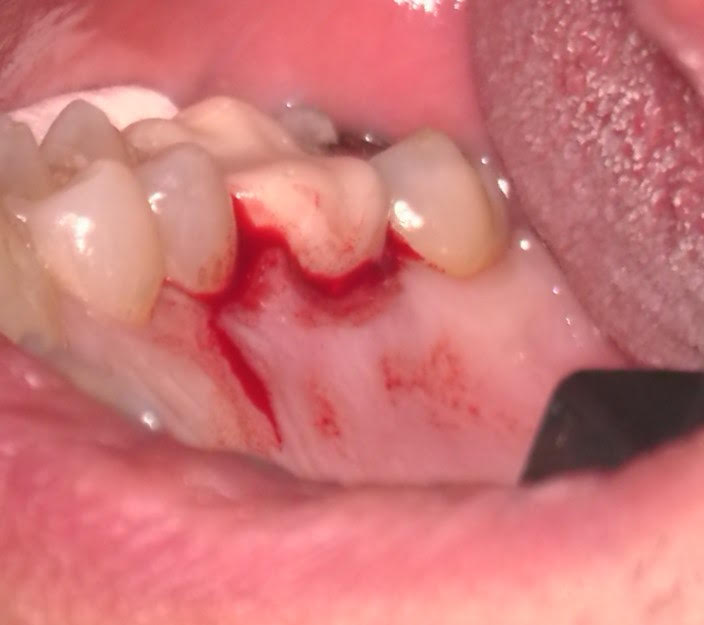
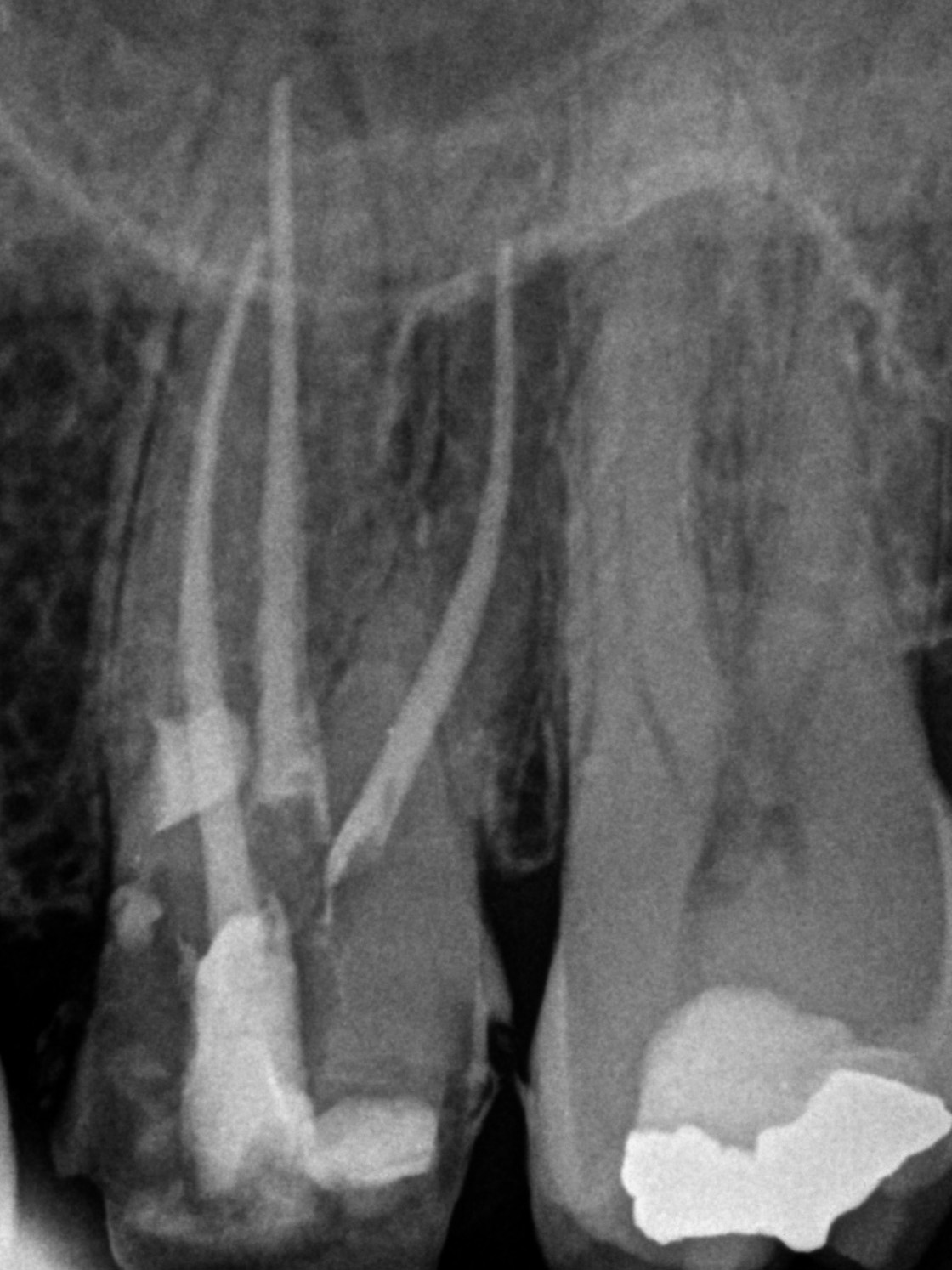
A 64-year-old male with a history of a fractured cusp on #14. He was asymptomatic, and his dentist placed a core buildup and provisional crown. However, the dentist noted that the fracture was very close to exposing the pulp. CBCT revealed cervical invasive external resorption on the mesio-palatal aspect of the palatal root, very close to the pulp. Due to the proximity of the fracture to the pulp, the need for a crown, and the resorptive defect, we recommended non-surgical RCT, followed by surgical resorption repair.
Treatment
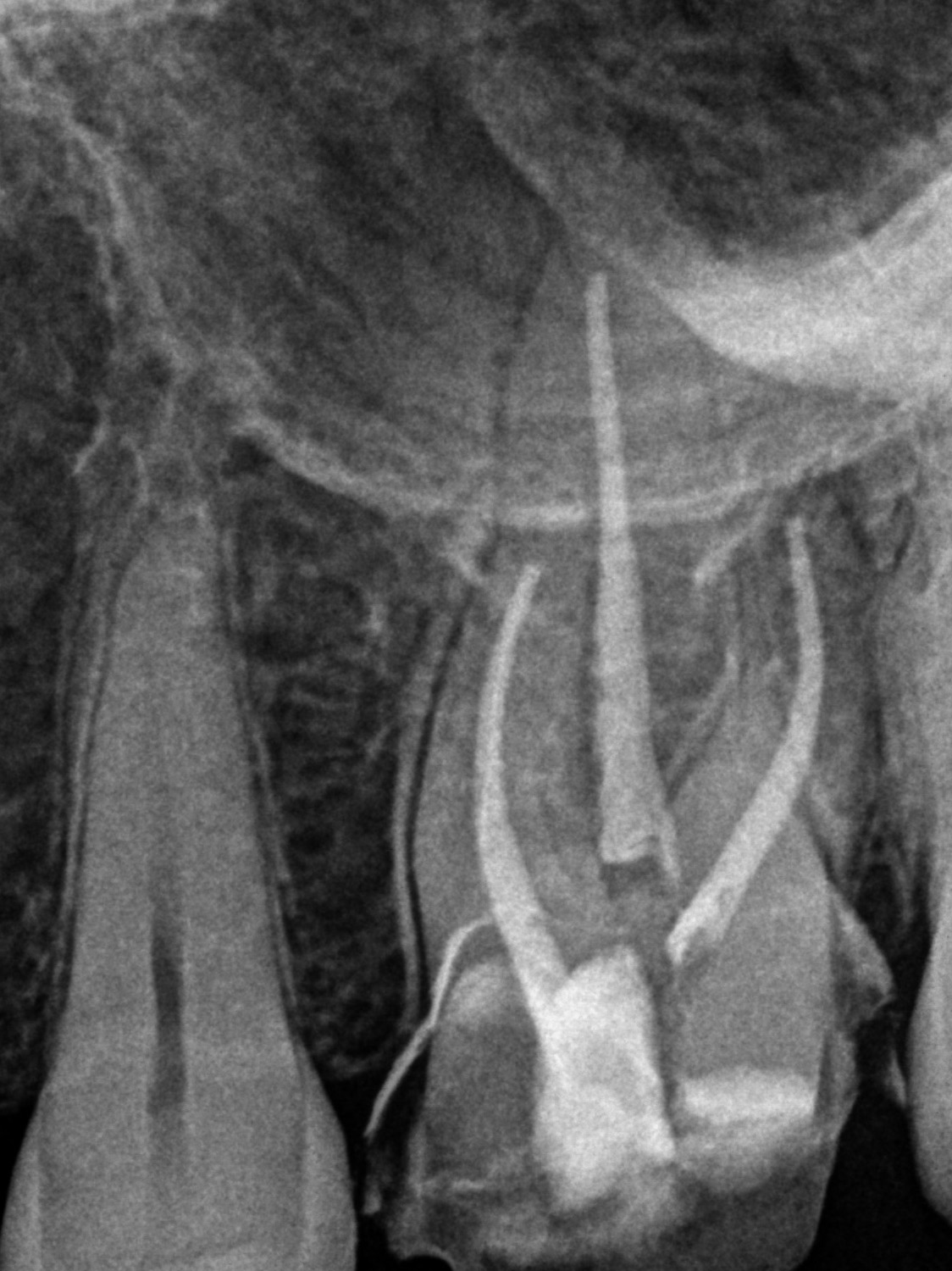
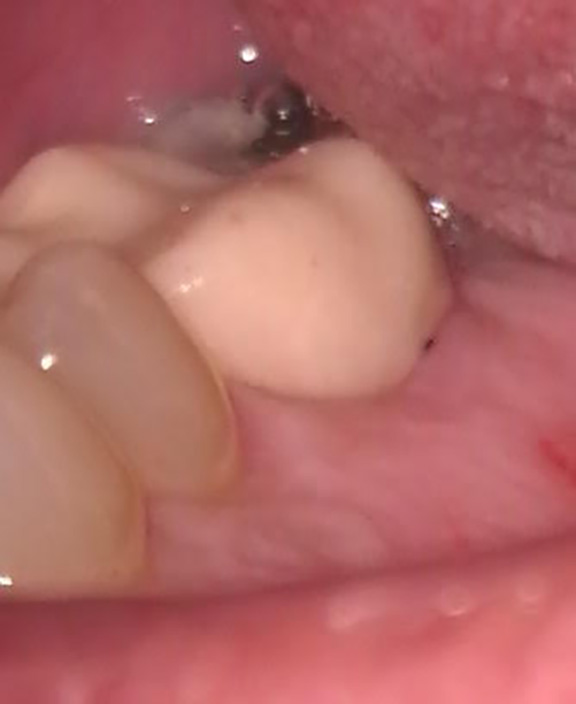
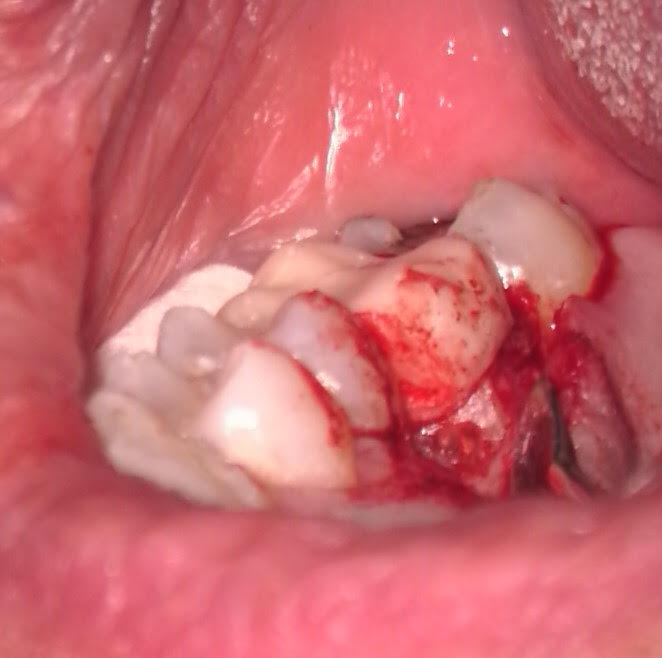
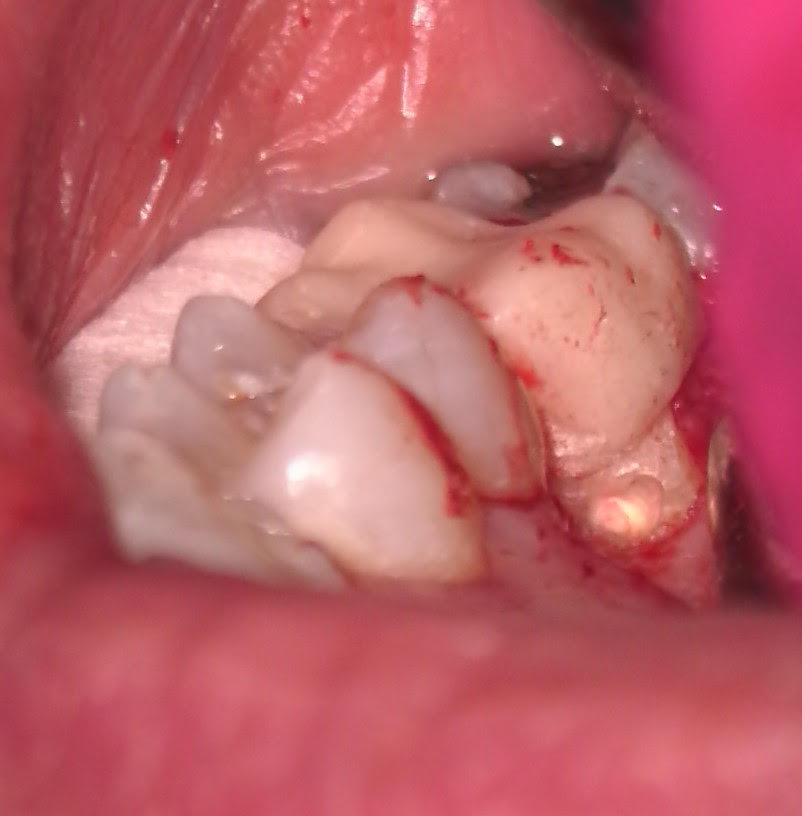
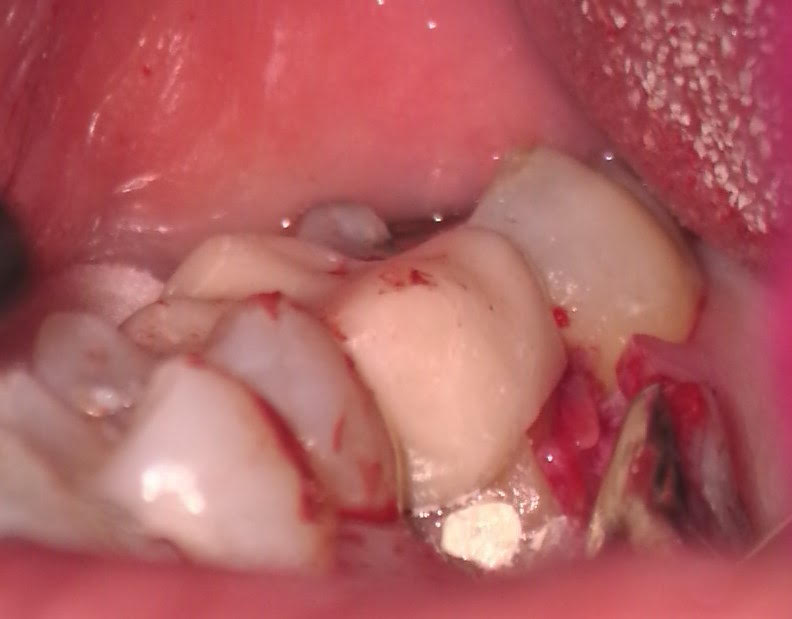
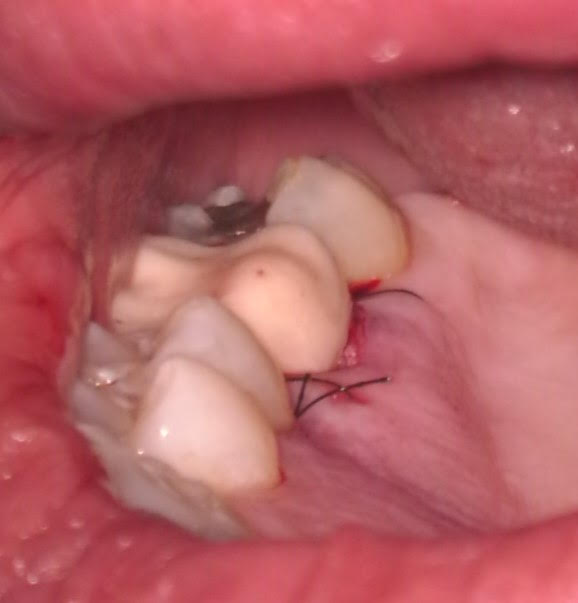
After removing the provisional crown, the root canal was completed using standard protocol (without Gentlewave) due to difficulty in achieving isolation. The patient returned a month later to surgically repair the resorptive defect. A palatal flap was performed with vertical releasing incision mesial to #13 to facilitate flap reflection and access to the area. Inflammatory granulation tissue was curetted from the defect which was then repaired with Bioceramic root repair material. A single suture was placed to reposition the flap. The tooth should have a favorable prognosis and the patient will proceed with the permanent crown in about 2 months.