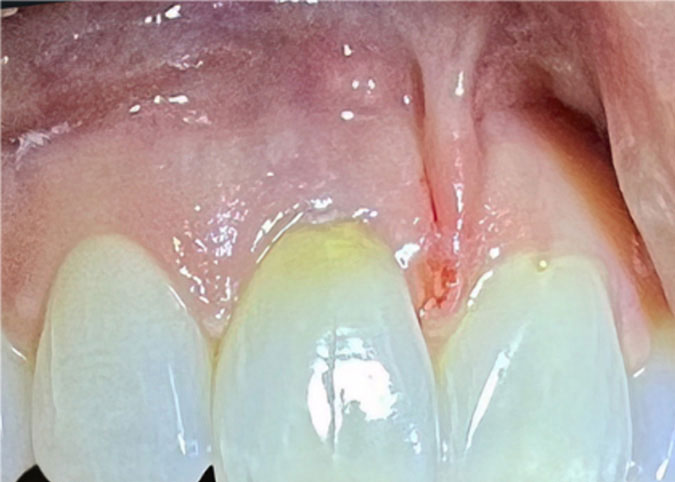
Until relatively recently, the etiology of resorption has been poorly understood and the ability to treat it has been limited, dooming many teeth to extraction. Once considered to be a rare condition, cervical invasive resorption seems to be on a dramatic rise. Thankfully, new technologies and materials have emerged which have greatly expanded our treatment options. Indeed, many of these teeth can be treated conservatively; some with surgery only, root canal only, or a combination of both treatments.
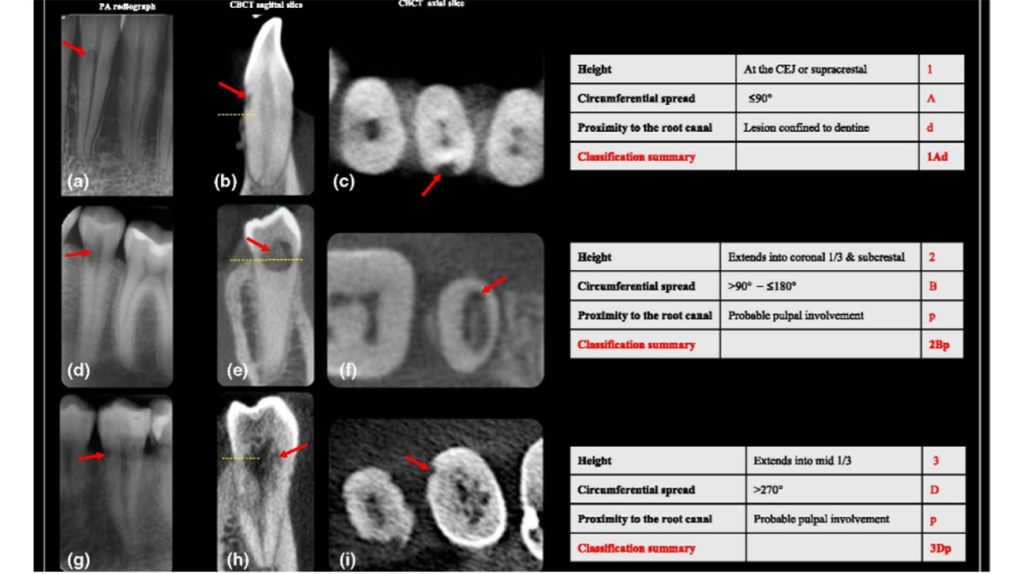
Successful treatment relies on a correct diagnosis. One of the most important developments in the predictable treatment of resorption has been the introduction of cone beam CT. For the first time, we are able to evaluate the true extent and location of the lesion three-dimensionally, allowing for more accurate diagnosis and more effective treatment planning. Critical elements to evaluate are:
- Location and extent of the lesion – is the lesion localized or does it spread circumferentially around the pulp?
- Is the pulp involved? If not, then surgery alone might be sufficient.
- Location and size of the portals of entry – is surgery necessary or would a root canal alone be effective?
Another challenge to overcome when treating external cervical resorption is the sub-gingival location of the defect. Traditional composites don’t bond well in a moist environment and have an unfavorable response when in contact with the pulp. In addition, they don’t allow for soft tissue reattachment, which could result in large periodontal defects. Therefore, even if we could access and clean the area, achieving an ideal seal and soft-tissue response has been unpredictable at best. However, new materials have emerged that allow for much more predictable outcomes. Bioceramics (e.g. BC Root Repair Material and Biodentin) have excellent biocompatibility and allow for cementum, bone, and PDL attachment. These materials are ideal when used below the level of the attachment and when the pulp is exposed. Geristore, a resin-modified glass ionomer, has also proven to be extremely effective in restoring these lesions and allows for the attachment of long-junctional epithelium and a favorable periodontal outcome.
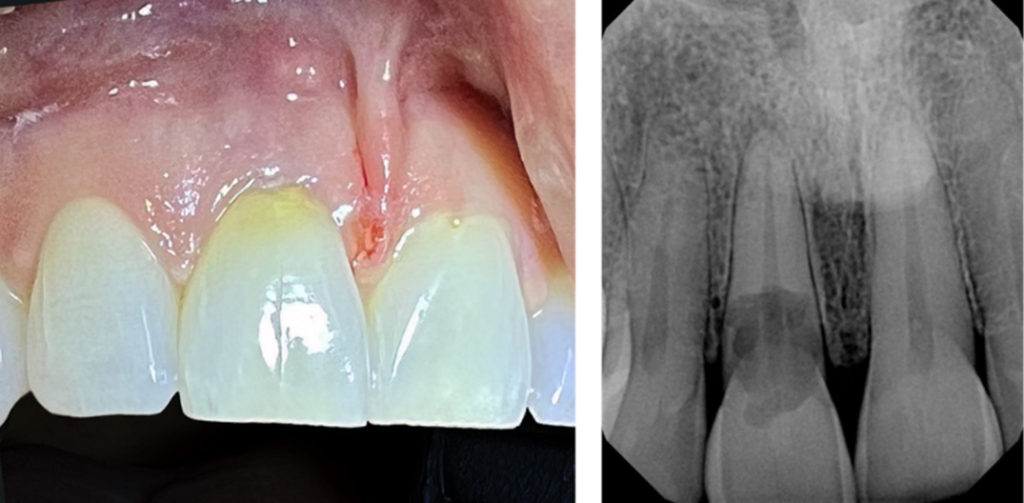
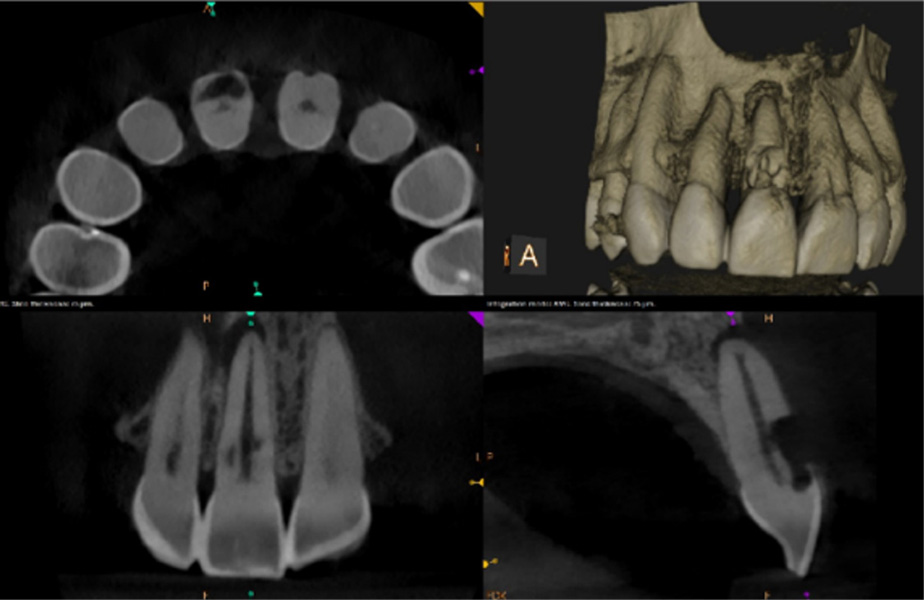
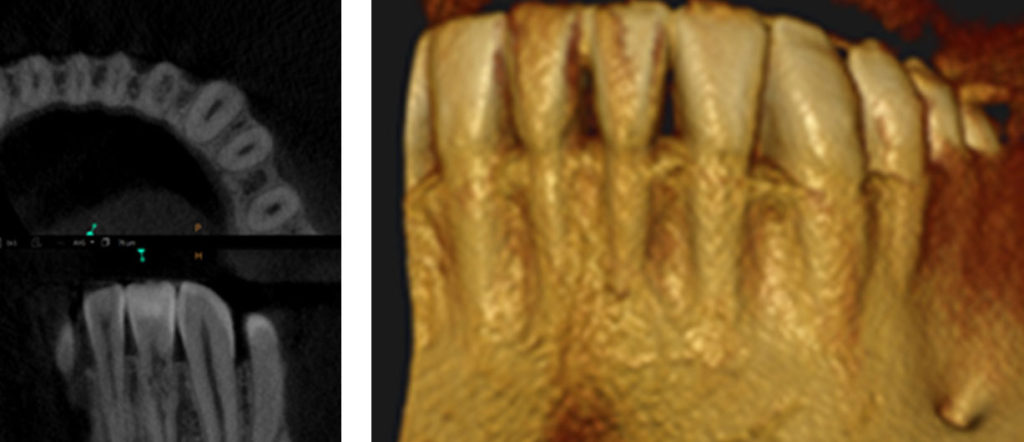
Case 1
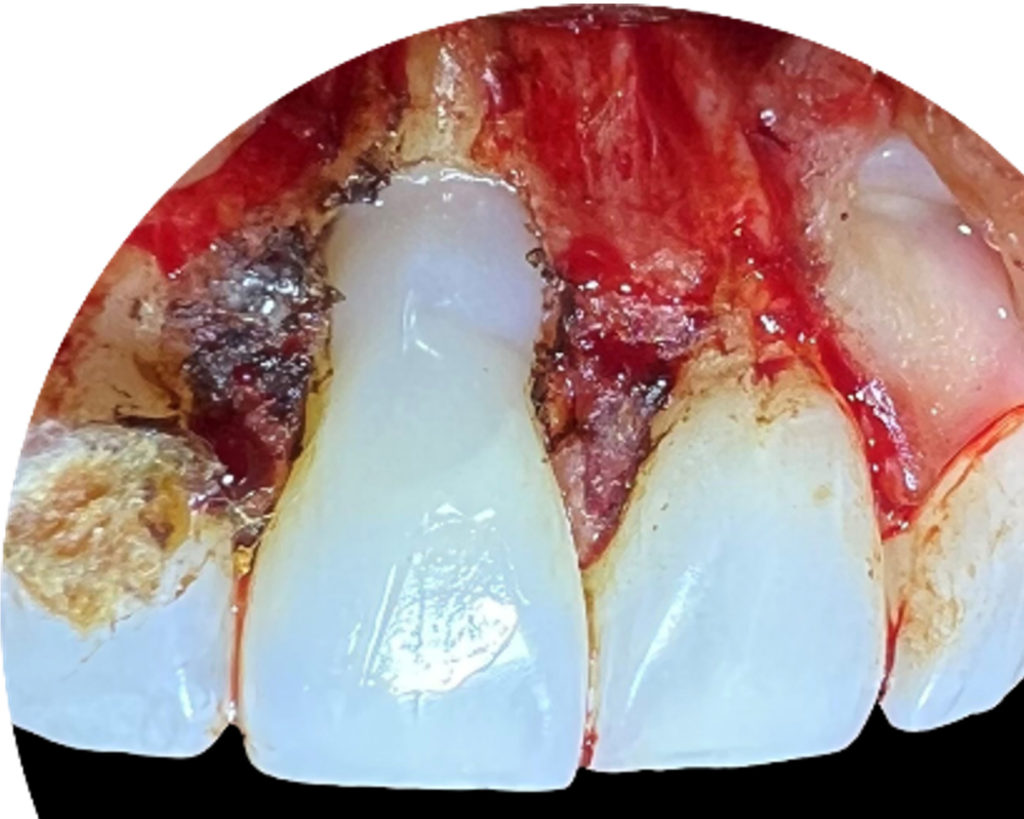
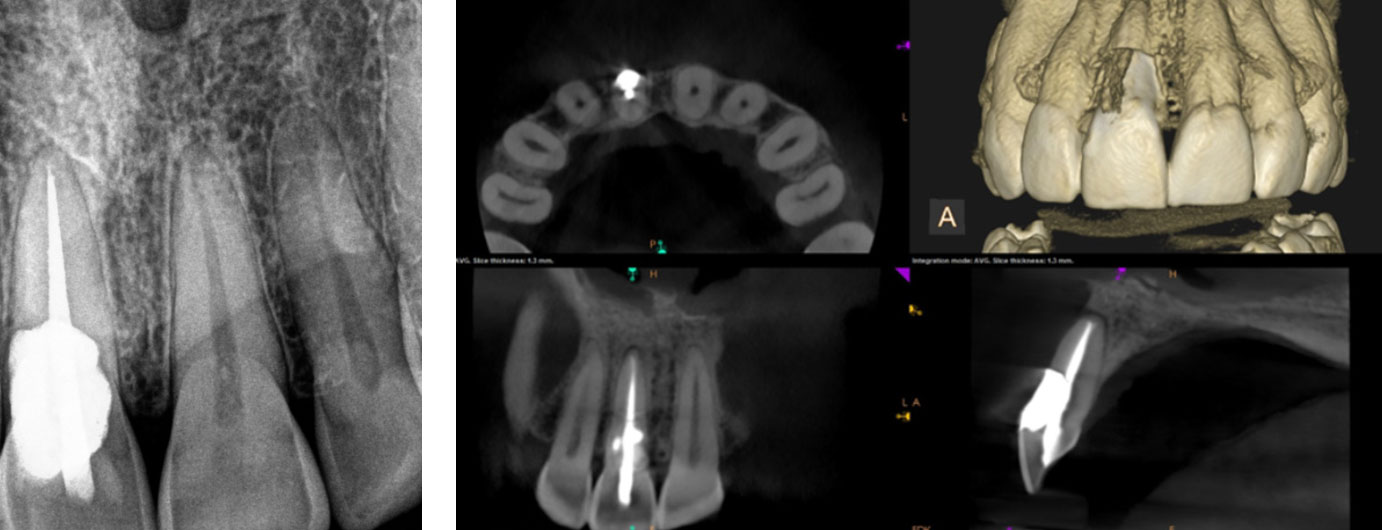
Large external resorptive defect, involving the pulp with apical lesion and bony fenestration. Root canal treatment was performed, followed by surgical repair with Geristore.
More extensive internal resorptive defects, however, have been very difficult to treat. These cases often have a highly irregular internal shape, often extending to the mid-root area or beyond, making traditional instrumentation difficult or impossible. They also often have multiple, small portals of entry that are not amenable to surgical intervention. Classically, these teeth had an unfavorable prognosis and were extracted. However, the novel Gentlewave procedure allows us to effectively clean these areas. Using apical negative pressure and multisonic frequency cleaning, it is now possible to clean these irregular and complex defects while still conserving dentin. We are then able to seal these defects using a highly flowable Bioceramic sealer.
Case 2
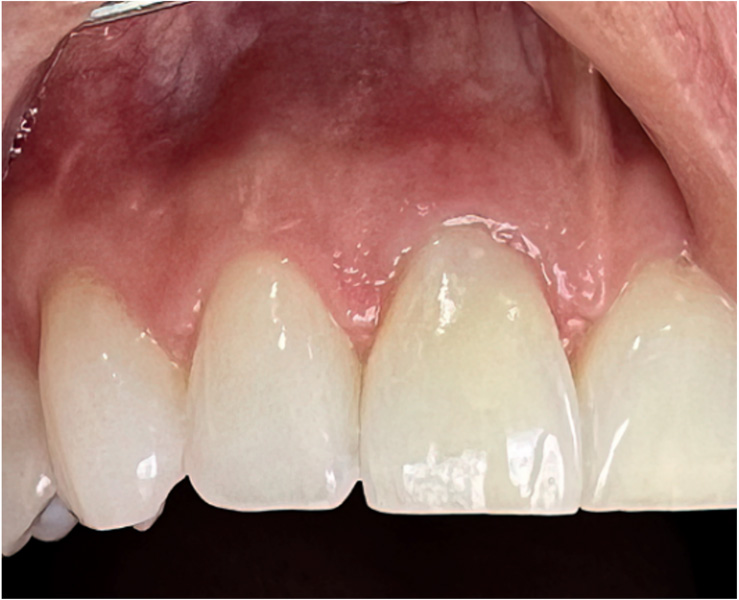
Complex internal resorption – the tooth was vital and asymptomatic.
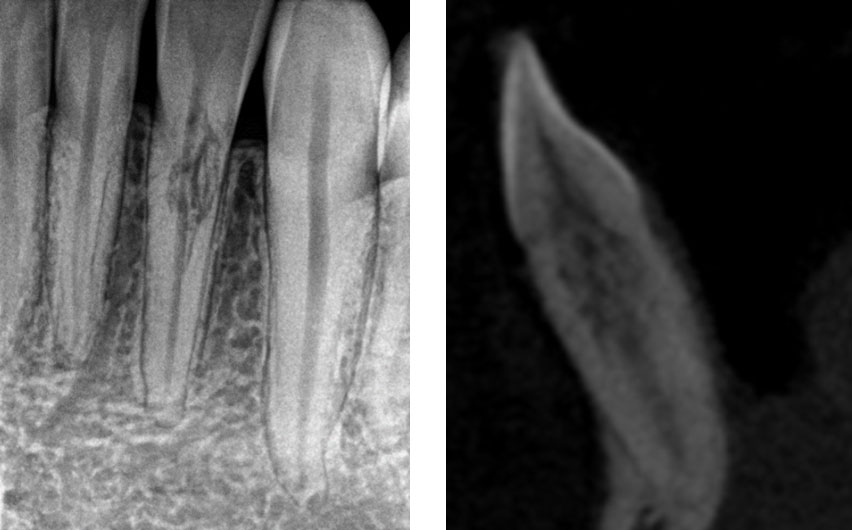
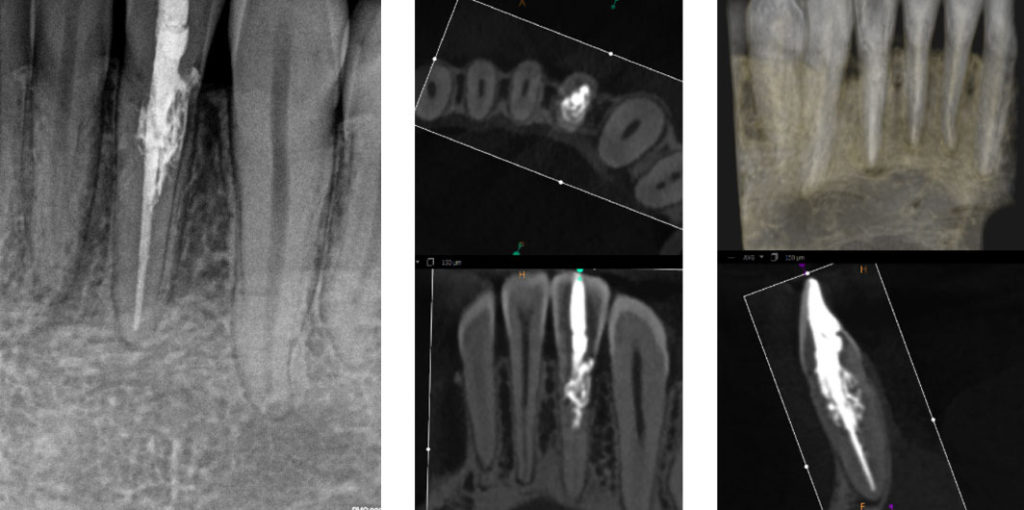
In summary, many, if not most teeth with cervical invasive resorption can now be predictably treated using conservative techniques. Surgical repair (with or without root canal treatment), and the Gentlewave procedure are often excellent treatment modalities and extraction should be now the treatment of last resort!